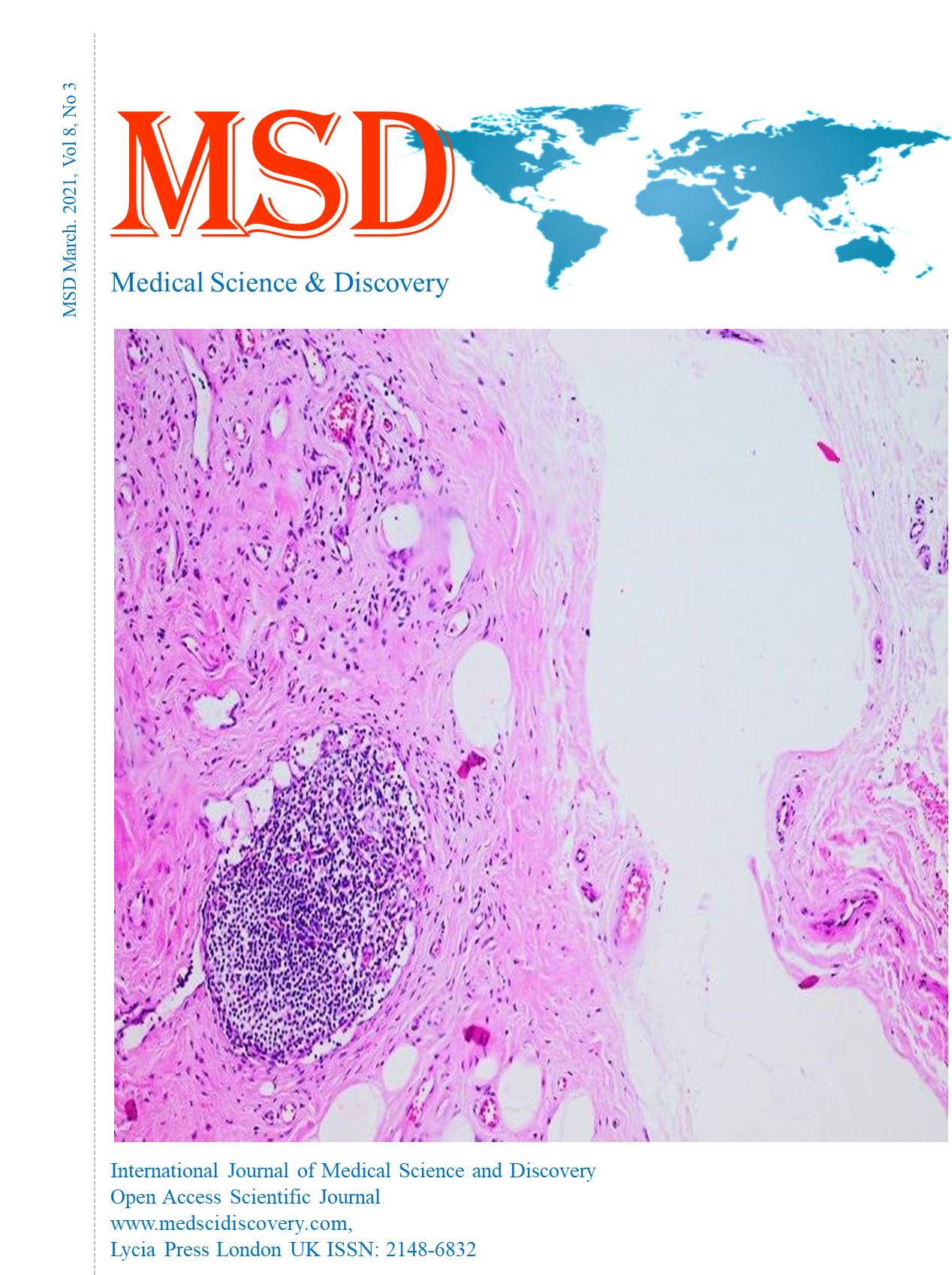
Investigation of the Value of Coagulation Parameters in Thromboembolic Events Among Patients Not Receiving Anticoagulant Therapy
Main Article Content
Abstract
Objective: The main causes of thromboembolic events are atherosclerosis, vascular endothelial injury, and hypercoagulability. Coagulation is activated through two basic mechanisms, including intrinsic and extrinsic pathways, leading to thrombin production as a result of a series of enzymatic reactions. The intrinsic pathway is evaluated with activated partial thromboplastin time (aPTT) and extrinsic pathway with prothrombin time (PT). This study aimed to investigate the relationship between thromboembolic diseases and coagulation parameters.
Material and Methods: Patients diagnosed with acute ischemic stroke (AIS) (n=216), acute coronary syndrome (ACS) (n=25), pulmonary thromboembolism (PTE) (n=15), and patients without an emergency pathology (n=71) (Control Group) in the emergency department were retrospectively reviewed in the period from 01 November 2016 to 31 March 2019.
Results: The aPTT (25.61±5.93 sec), PT (12.05±2.26 sec), and INR (1.04±0.19) values of the AIS group were statistically significantly lower compared to values of the control group (p = ˂0.001, ˂0.001 and ˂0.001 respectively). Similarly, the aPTT (27.15±8.97 sec), PT (12.26±2.75 sec), and INR (1.03±0.25) values of the ACS group were statistically significantly lower compared to those of the control group (p=0.012, 0.030, and 0.001, respectively). There was no statistically significant difference between the PTE group and control group in terms of aPTT, PT, and INR values (p= 0.133, 0.758, and 0.711, respectively).
Conclusion: Shortened aPTT levels in cases without a history of anticoagulant use at the time of admission can be considered to be a predictive and effective tool for clinicians in arterial embolic events (AIS and ACS).
Downloads
Article Details
Accepted 2021-03-15
Published 2021-03-28
References
2.Koster T, Vandenbroucke JP, Rosendaal FR, Briët E, Rosendaal FR, Blann AD. Role of clotting factor VIII in effect of von Willebrand factor on occurrence of deep-vein thrombosis. Lancet 1995 Jan;345(8943):152–5.
3.Vlieg A van H, van der Linden IK, Bertina RM, Rosendaal FR. High levels of factor IX increase the risk of venous thrombosis. Blood 2000 Jun 15;95(12):3678–82.
4.Korte W, Clarke S, Lefkowitz JB. Short Activated Partial Thromboplastin Times Are Related to Increased Thrombin Generation and an Increased Risk for Thromboembolism. Am J Clin Pathol 2000 Jan 1;113(1):123–7.
5.Tripodi A, Chantarangkul V, Martinelli I, Bucciarelli P, Mannucci PM. A shortened activated partial thromboplastin time is associated with the risk of venous thromboembolism. Blood 2004 Dec 1;104(12):3631–4.
6.Sotoudeh Anvari M, Tavakoli M, Lotfi-Tokaldany M, Broumand M, Rezahosseini O, Hakki-Kazzazi E, et al. Coronary artery disease presentation and its association with shortened activated partial thromboplastin time. J Tehran Univ Hear Cent. 2018 Jan;13(1):1-5.
7.Abdullah WZ, Moufak SK, Yusof Z, Mohamad MS, Kamarul IM. Shortened activated partial thromboplastin time, a hemostatic marker for hypercoagulable state during acute coronary event. Transl Res . 2010 Jun;155(6):315–9.
8.Prandoni P. Venous thromboembolism and atherosclerosis: Is there a link? J Thromb Haemost. 2007 Jul;5 Suppl 1:270-5.