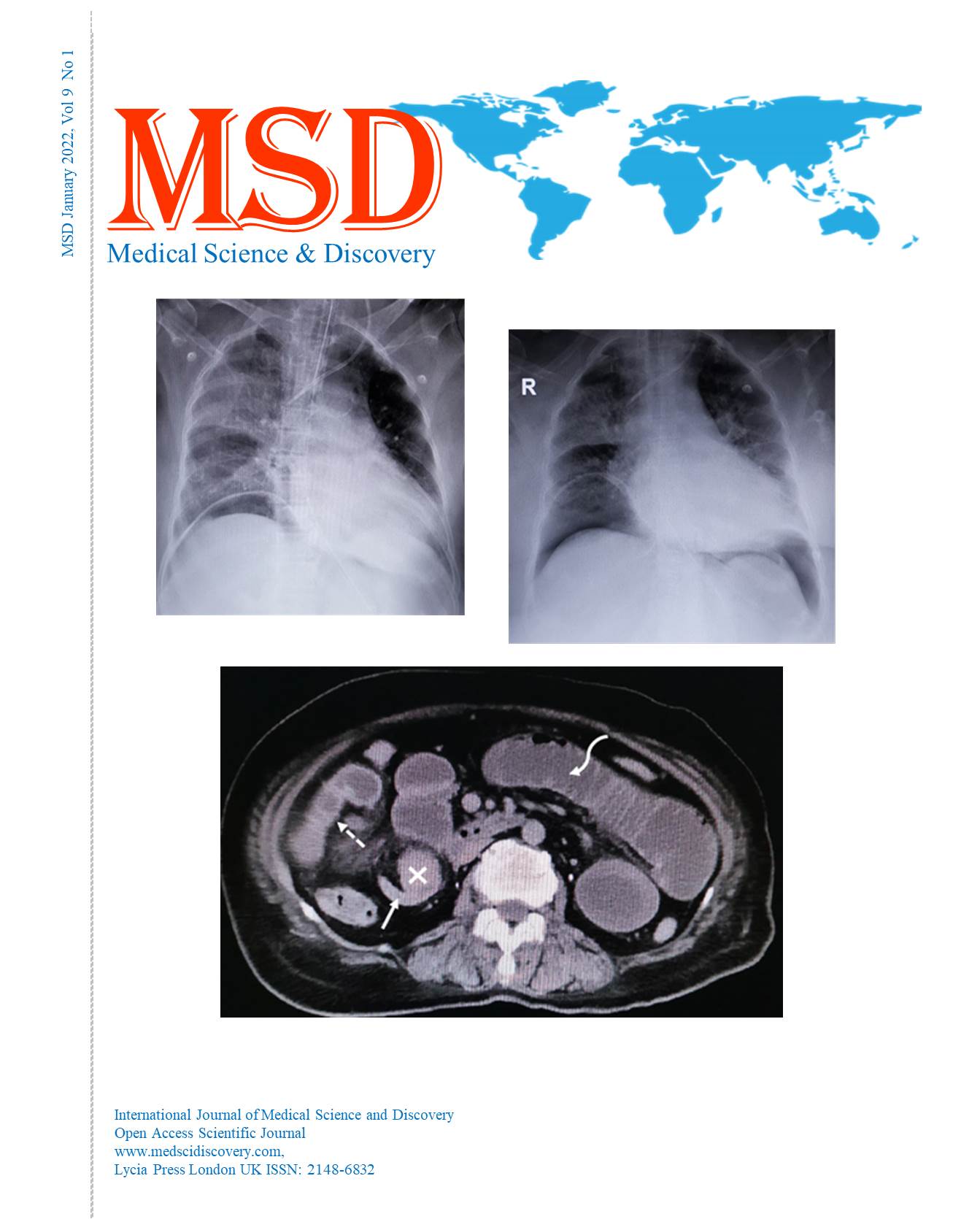
Effects of EGFR gene mutation on stage 3A lung adenocarcinomas in the clinical decision-making process for mediastinal invasive staging
Main Article Content
Abstract
Objective: In our study, we aimed to evaluate the effects of EGFR gene mutation on the clinical course of Non-Small Cell Lung carcinoma.
Material and Methods: Our study was conducted retrospectively on patients who were operated on for NSCLC diagnosed as adenocarcinoma. The International Cancer Control Association and the American Cancer Committee eighth TNM classification system were evaluated in our study. Case groups at this stage were divided into two main groups as EGFR gene mutation (+/-) and data between the clinical behaviours of these two main groups were investigated.
Results: There was no statistically significant difference between the two groups in terms of age, gender, smoking, and type of surgery (p = 0.727, p = 0.936, p = 0.463). The relationship between EGFR and surgery type was also not significant (2 = 0.268; p = 0.992). There were no statistically significant difference between the medians of Suv-Max value (z = 1.083; p = 0.279). Among 653 cases in all NSCLC adenocarcinoma subtypes, EGFR gene mutation positivity was 23.89%. When we evaluate the progression of patients with EGFR gene mutation from stage 3A to 3B, it is more aggressive in cases with EGFR gene mutation, but it is not statistically significant (c2=2.924; p=0.087).
Conclusions: Knowledge of whether there is an EGFR gene mutation can provide important clinical information. In this respect, EGFR gene mutation positivity in stage 3A cases may constitute an indication for preoperative invasive mediastinal sampling, but we need more data to get statistically definitive results.
Downloads
Article Details

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
Accepted 2022-01-14
Published 2022-01-24
References
Spiro SG, Porter JC. Lung cancer-where are we today? Current advances in staging and nonsurgical treatment. Am J Respir Crit Care Med 2002;166:1166–96. DOI: https://doi.org/10.1164/rccm.200202-070SO
Gazdar AF. Activating and resistance mutations of EGFR in non-small-cell lung cancer: role in clinical response to EGFR tyrosine kinase inhibitors. Oncogene. 2009 Aug;28 Suppl 1:S24-31. DOI: https://doi.org/10.1038/onc.2009.198
Lynch TS, Bell DW, Sordella R, et al. Activating mutations in the EGFR underlying responsiveness of NSCLC to gefitinib. N Engl J Med 2004; 350:2129-39. DOI: https://doi.org/10.1056/NEJMoa040938
Rosell R, Carcereny E, Gervais R, et al. Erlotinib versus standard chemotherapy as first-line treatment for European patients with advanced EGFR mutation-positive non-small-cell lung cancer (EURTAC): a multicentre, open-label, randomized phase 3 trial. Lancet Oncol 2012;13:239-246. DOI: https://doi.org/10.1016/S1470-2045(11)70393-X
Paez JG, Jänne PA, Lee JC, et al. EGFR mutations in lung cancer: correlation with clinical response to gefitinib therapy. Science 2004;304:1497-1500. DOI: https://doi.org/10.1126/science.1099314
V. Rusch et al.Differential Expression of the Epidermal Growth Factor Receptor and Its Ligands in Primary Non-Small Cell Lung Cancers and Adjacent Benign Lung. (CANCER RESEARCH 53. 2379-2385. May 15.
Sharma SV1, Bell DW, Settleman J, Haber DA. Epidermal growth factor receptor mutations in lung cancer. Nat Rev Cancer. 2007 Mar;7(3):169-81. DOI: https://doi.org/10.1038/nrc2088
Watanabe H, Okauchi S, Miyazaki K, Satoh H, Hizawa N. Factors Associated With Distant Metastasis in EGFR-mutated Non-small Cell Lung Cancer Patients: Logistic Analysis. In Vivo. 2019;33(4):1369-1372. DOI: https://doi.org/10.21873/invivo.11613
Togashi Y, Masago K, Kubo T, et al. Association of diffuse, random pulmonary metastases, including miliary metastases, with epidermal growth factor receptor mutations in lung adenocarcinoma. Cancer. 2011;117(4):819-825. DOI: https://doi.org/10.1002/cncr.25618
Akif Turna et al. The eighth staging system of non-small cell lung cancer and its practical implications. Turk Gogus Kalp Dama 2017;25(3):484-498. DOI: https://doi.org/10.5606/tgkdc.dergisi.2017.14362
Öztaş S et al. The role of tumor SUVmax/lymph node SUVmax ratio viewed on PET-CT in the detection of mediastinal metastasis in patients with lung cancer. Turk Gogus Kalp Dama 2012;20:544-551. DOI: https://doi.org/10.5606/tgkdc.dergisi.2012.103
Mountain CF, Dresler CM. Regional lymph node classification for lung cancer staging. Chest 1997;111:1718-1723. DOI: https://doi.org/10.1378/chest.111.6.1718
Li AR, Chitale DA, Riely GJ, Pao W, Miller VA, Zakowski MF, et al. EGFR mutations in lung adenocarcinomas: clinical testing experience and relationship to EGFR gene copy number and immunohistochemical expression. J Mol Diagn 2008;10:242-8. DOI: https://doi.org/10.2353/jmoldx.2008.070178
Jiang G, Fan C, Zhang X, et al. Ascertaining an appropriate diagnostic algorithm using EGFR mutation-specific antibodies to detect EGFR status in non-small-cell lung cancer. PLoS One. 2013;8(3):e59183. DOI: https://doi.org/10.1371/journal.pone.0059183
Yoneda K, Imanishi N, Ichiki Y, Tanaka F. Treatment of Non-small Cell Lung Cancer with EGFR-mutations. J UOEH. 2019;41(2):153-163. doi:10.7888/juoeh.41.153 DOI: https://doi.org/10.7888/juoeh.41.153
Zhang H, Chen J, Liu T, Dang J, Li G. First-line treatments in EGFR-mutated advanced non-small cell lung cancer: A network meta-analysis. PLoS One. 2019;14(10):e0223530. DOI: https://doi.org/10.1371/journal.pone.0223530
Leighl NB, Rekhtman N, Biermann WA, et al. Molecular testing for selection of patients with lung cancer for epidermal growth factor receptor and anaplastic lymphoma kinase tyrosine kinase inhibitors: American Society of Clinical Oncology endorsement of the College of American Pathologists/International Association for the study of lung cancer/association for molecular pathology guideline. J Clin Oncol. 2014;32(32):3673-3679. DOI: https://doi.org/10.1200/JCO.2014.57.3055
Pirker R, Herth JF, Kerr KM, et al. Consensus for EGFR mutation testing in non-small cell lung cancer: results from a European workshop. J Thorac Oncol 2010;5:1706-13. DOI: https://doi.org/10.1097/JTO.0b013e3181f1c8de
Scott WJ, Howington J, Feigenberg S, Movsas B, Pisters K; American College of Chest Physicians. Treatment of non-small cell lung cancer stage I and stage II: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3 Suppl):234S-242S. DOI: https://doi.org/10.1378/chest.07-1378
Molina JR, Yang P, Cassivi SD, Schild SE, Adjei AA. Non-small cell lung cancer: epidemiology, risk factors, treatment, and survivorship. Mayo Clin Proc. 2008;83(5):584-594. DOI: https://doi.org/10.1016/S0025-6196(11)60735-0
Liam CK, Andarini S, Lee P, Ho JC, Chau NQ, Tscheikuna J. Lung cancer staging now and in the future. Respirology. 2015;20(4):526-534. DOI: https://doi.org/10.1111/resp.12489
Silvestri GA, Gonzalez AV, Jantz MA, et al. Methods for staging non-small cell lung cancer: Diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest. 2013;143(5 Suppl):e211S-e250S. DOI: https://doi.org/10.1378/chest.12-2355
Kim CH, Kim SH, Park SY, Yoo J, Kim SK, Kim HK. Identification of EGFR Mutations by Immunohistochemistry with EGFR Mutation-Specific Antibodies in Biopsy and Resection Specimens from Pulmonary Adenocarcinoma. Cancer Res Treat. 2015;47(4):653-660. DOI: https://doi.org/10.4143/crt.2014.118
Rosell R, Moran T, Queralt C, Porta R, Cardenal F, Camps C, et al.
Screening for epidermal growth factor receptor mutations in lung cancer. N Engl J Med 2009;361:958–67. DOI: https://doi.org/10.1056/NEJMoa0904554
Midha A, Dearden S, McCormack R. EGFR mutation incidence in non-small-cell lung cancer of adenocarcinoma histology: a systematic review and global map by ethnicity (mutMapII). Am J Cancer Res. 2015;5(9):2892-2911. Published 2015 Aug 15.
Calibasi-Kocal G, Amirfallah A, Sever T, et al. EGFR mutation status in a series of Turkish non-small cell lung cancer patients. Biomed Rep. 2020;13(2):2. doi:10.3892/br.2020.1308 DOI: https://doi.org/10.3892/br.2020.1308
Castellanos E, Feld E, Horn L. Driven by Mutations: The Predictive Value of Mutation Subtype in EGFR-Mutated Non-Small Cell Lung Cancer. J Thorac Oncol. 2017;12(4):612-623. DOI: https://doi.org/10.1016/j.jtho.2016.12.014
Wang Y, Yang N, Zhang Y, et al. Effective Treatment of Lung Adenocarcinoma Harboring EGFR-Activating Mutation, T790M, and cis-C797S Triple Mutations by Brigatinib and Cetuximab Combination Therapy. J Thorac Oncol. 2020;15(8):1369-1375. DOI: https://doi.org/10.1016/j.jtho.2020.04.014
Zhang YL, Yuan JQ, Wang KF, et al. The prevalence of EGFR mutation in patients with non-small cell lung cancer: a systematic review and meta-analysis. Oncotarget. 2016;7(48):78985-78993. DOI: https://doi.org/10.18632/oncotarget.12587