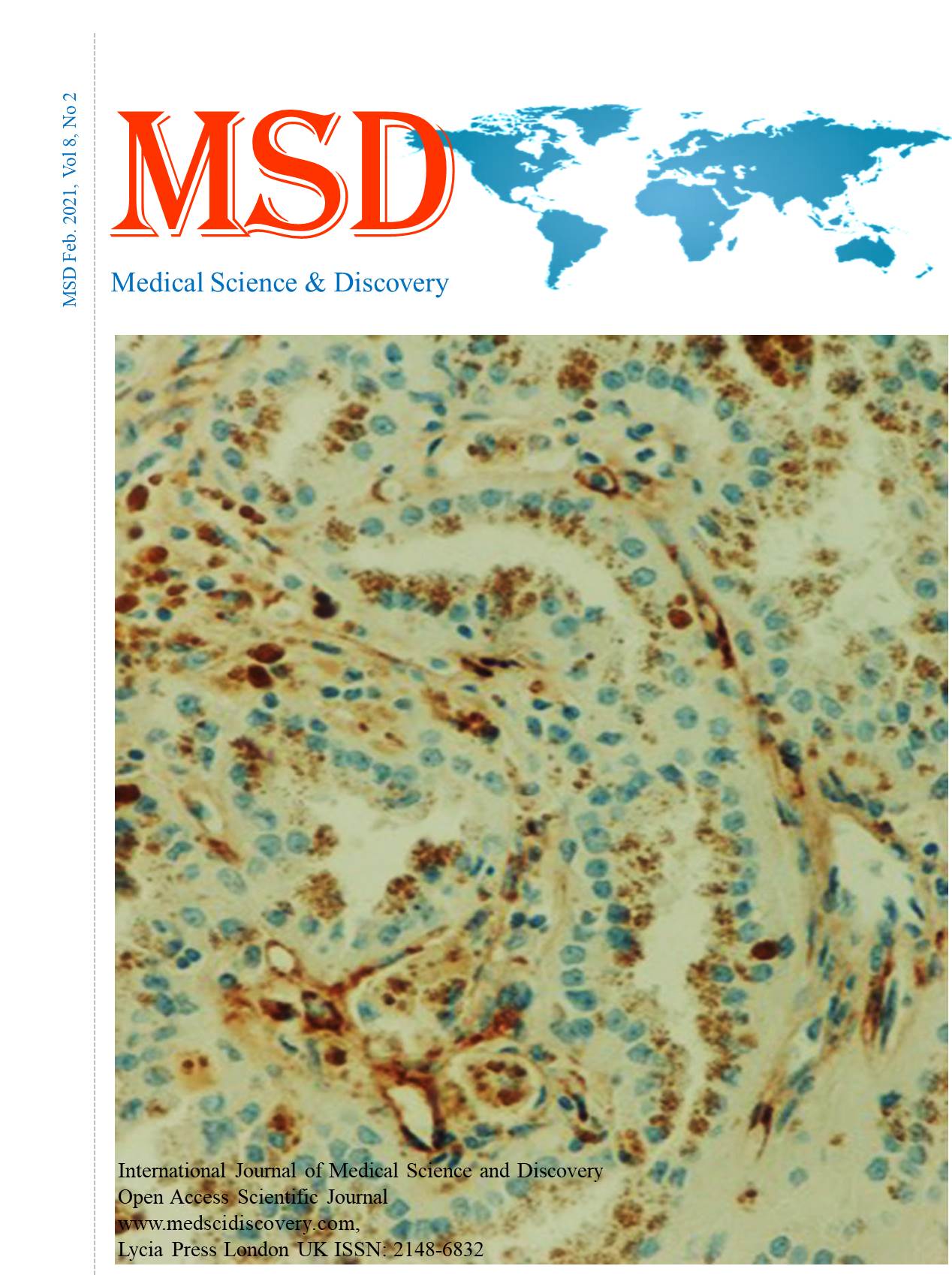
Second Branchial Cleft Cyst: A Case Report Branchial Cleft Cyst
Main Article Content
Abstract
Objective: Branchial anomalies are congenital pathologies that are seen in the lateral region of the neck and are generally benign. The branchial clefts develop in the 2nd-7th weeks of fetal life as embryonal development. The branchial anomalies are caused by non-disappearance, abnormal development and, incomplete emerger of the branchial clefts and pockets during embryonal development. The branchial anomalies are generally seen as the cyst. The most common cyst was the second branchial cleft cyst with 95%. Their diameter is usually a few centimeters.
Case: A 37-year old male patient was admitted to the hospital because of a swelling on the left side of his neck for four years. Physical examination revealed a mobile cystic mass in level 2 at the upper left jugular region of the neck. The cystic mass and the surrounding lymph nodes were excised and sent to the pathology laboratory. A cystic mass, approximately 5x4x3.5 cm in size, containing cystic areas was observed macroscopically. Microscopically, the cyst was lined with squamous epithelium and contained large lymphocyte groups in the subepithelial area. The case was reported as the branchial cleft cyst.
Conclusion: Branchial cleft cysts should be excised before reaching large sizes, as they may cause pain and pressure on the surrounding tissue. In addition, it should be kept in mind that malignancy may develop from branchial cleft cysts, although rare.
Downloads
Article Details
Accepted 2021-02-18
Published 2021-02-24
References
Koç C. Otorhinolaryngology and head-neck surgery. Ankara: Güneş Bookstore 2004;891
Pınarbaşlı MO, Ture N, Kaya E, Arık D, Gurbuz MK. Squamous cell carcinoma developed on the basis of branchial cyst (Primary branchiogenic carcinoma). Pamukkale Medical Journal 2014;7(3):240-244
Hart C, Opperman D, Gulbahce E, Adams G. Branchial cleft cyst: a rare diagnosis in a 91-year-old patient. Otolaryngol Head Neck Surg 2006;135:955-977
Ohri AK, Makins R, Smith CE, Leopold PW. Primary branchial cleft carcinoma-a case report. J Laryngol Otol 1997;111(1):80-82
Glosser JW, Pires CA, Feinberg SE. Branchial cleft or cervical lymphoepithelial cysts: etiology and management. J Am Dent Assoc 2003;134(1):81-86
Mandell DL. Head and neck anomalies related to the branchial apparatus. Otolaryngol Clin North Am 2000;33:1309-1332
Wasson J, Blaney S, Sımo R. A third branchial pouch cyst presenting as stridor in a child. Ann R Coll Surg Engl 2007;89(1):W12-14
Okur E, Okur N, Yücedag F, Ayçiçek A, Aktepe Üçüncü F. Journal of ear nose throat
and head neck surgery. Third Branchial Cleft Anomaly: A Case Report 2011;19(3):160-163
Kim MG, Lee NH, Ban JH, Lee KC, Jin SM, Lee SH. Sclerotherapy of branchial cleft cyst using OK-432. Otolaryngol Head Neck Surg 2009;141:329-334
Thomaidis V, Seretis K, Tamiolakis D, Papadopoulos N, Tsamis I. Branchial cysts. A report of 4 cases. Acta Dermatovenerol. Alp. Panonica Adriat 2006;15:85-89
Houck J. Excision of branchial cysts. Operative Tech Otolaryngol 2005;16(3):213-222
Daoud FS. Branchial cyst: an often forgotten diagnosis. Asian J Surg 2005;28(3):174-178
Tansuker HD, Coşkun BU, Sozen ME, Başak T, Dadaş B. [Branchial cleft cyst: a rare diagnosis in a 84-year old patient. A case report]. Turk Arch Otolaryngol 2011;49(1):22-24
Maturo SC, Michaelson PG, Faulkner JA. Primary branchiogenic carcinoma: the confusion continues. Am J Otolaryngol 2007;28(1):25-27
Telander R, Filston H, Review of head and neck lesions in infancy and childhood. Surg Clin North Am 1992;72:1429-1447
Alimoğlu Y, Altın F. Second Branchial Cleft Anomalies: Analysis of Our Clinical Experience in 10 Years. KBB-Forum 2020;19(1):22-26