Artificial intelligence in the endocrine clinic: automated bone age analysis in arabic children from UAE Artificial intelligence in bone age analysis
Main Article Content
Abstract
Objective: Artificial intelligence (AI) is playing an increasing role in patient assessment. AI bone age analysis is such a tool, but its value in Arabic children presenting to an endocrine clinic has not been explored. We compared results from an experienced pediatric radiologist and the AI bone age system, BoneXpert (BX), (Visiana, Denmark) to assess its utility in a cohort of children presenting to the Al Jalila Children’s Specialty Hospital endocrine service.
Materials and Methods: We conducted a retrospective chart review of 47 children with growth disorders, initially assessed by a single experienced radiologist and subsequently by BX, to confirm the usefulness of the BX system in our population. The results of the analyses were analysed using a Bland-Altman plot constructed to compare differences between the radiologist’s interpretation and BX across the available range of bone age.
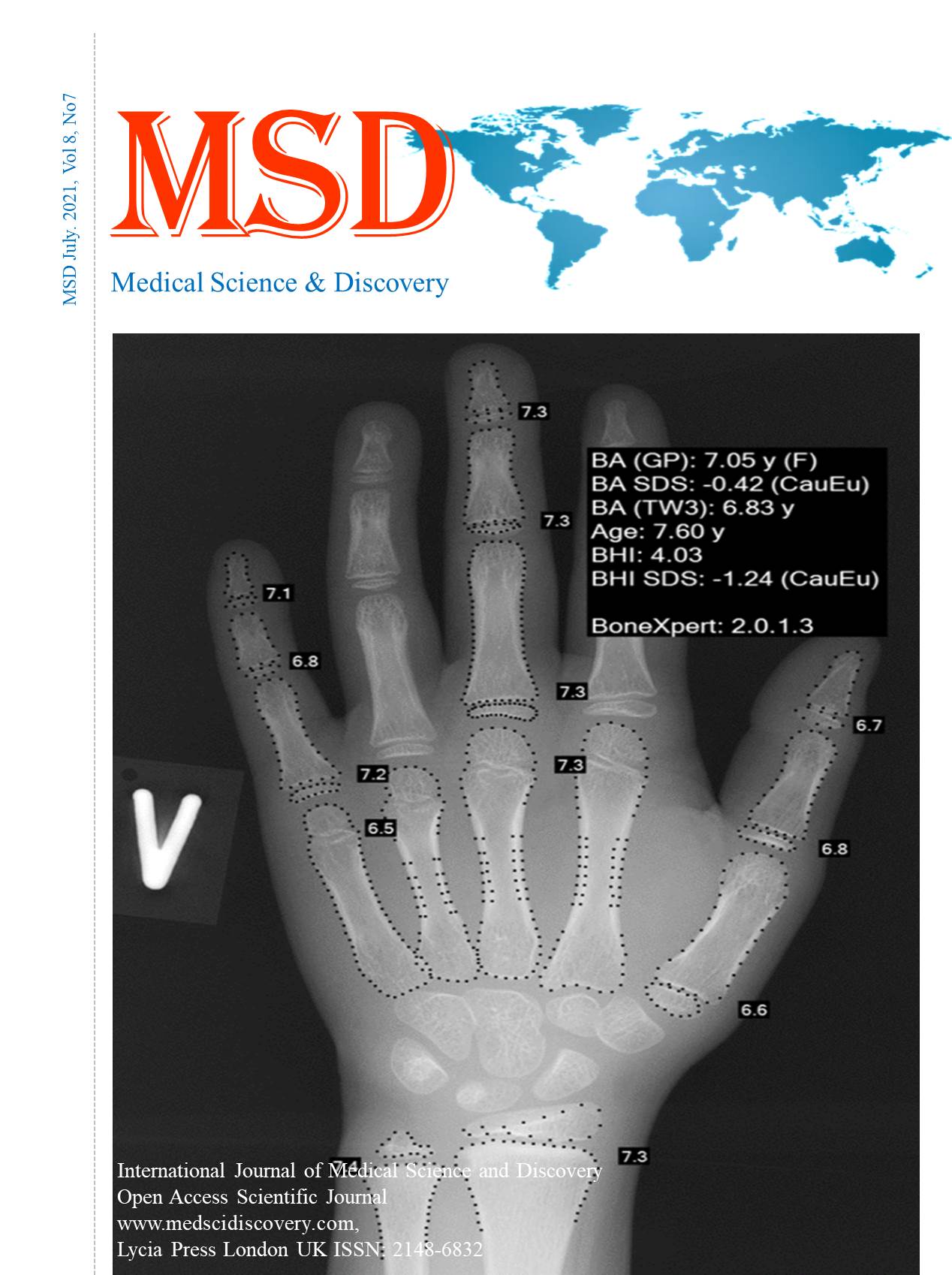
Results: Forty-four of the patient x-ray images were analysed by BX. Three X-ray images were rejected by BX due to post-processing artifacts, which prevented computer interpretation. For the remaining 44 X-rays, there was a close correlation between radiologist and BX results (r=0.93; p <0.00001). Two radiographs were identified with a large discrepancy in the reported bone ages. Blinded, independent re-evaluation of the radiographs showed the original manually interpreted bone age to have been erroneous, with the BX results corresponding closely to the amended bone age. A small positive bias was noted in bone age (+0.39 years) in the BX analyses, relative to manual interpretation.
Conclusions: AI bone age analysis was of high utility in Arabic children from UAE presenting to an endocrine clinic, with results highly comparable to an experienced radiologist. In the two cases where a large discrepancy was found, independent re-evaluation showed AI analysis was correct.
Downloads
Article Details
Accepted 2021-07-20
Published 2021-07-28
References
Creo AL, Schwenk WF 2nd. Bone Age: A Handy Tool for Pediatric Providers. Pediatrics. 2017 Dec;140(6):e20171486. https://doi.org/10.1542/peds.2017-1486 PMID:29141916
Martin DD, Wit JM, Hochberg Z, Sävendahl L, van Rijn RR, Fricke O, et al. The use of bone age in clinical practice - part 1. Horm Res Paediatr. 2011;76(1):1–9. https://doi.org/10.1159/000329372 PMID:21691054
Labarta JI, Ranke MB, Maghnie M, Martin D, Guazzarotti L, Pfäffle R, et al. Important Tools for Use by Pediatric Endocrinologists in the Assessment of Short Stature. J Clin Res Pediatr Endocrinol. 2021 Jun;13(2):124–35. https://doi.org/10.4274/jcrpe.galenos.2020.2020.0206 PMID:33006554
Vargas Trujillo M, Dragnic S, Aldridge P, Klein KO. Importance of individualizing treatment decisions in girls with central precocious puberty when initiating treatment after age 7 years or continuing beyond a chronological age of 10 years or a bone age of 12 years. J Pediatr Endocrinol Metab. 2021 Apr;34(6):733–9. https://doi.org/10.1515/jpem-2021-0114 PMID:33856747
Martin DD, Schittenhelm J, Thodberg HH. Validation of adult height prediction based on automated bone age determination in the Paris Longitudinal Study of healthy children. Pediatr Radiol. 2016 Feb;46(2):263–9. https://doi.org/10.1007/s00247-015-3468-8 PMID:26573823
Martin DD, Wit JM, Hochberg Z, van Rijn RR, Fricke O, Werther G, et al. The use of bone age in clinical practice - part 2. Horm Res Paediatr. 2011;76(1):10–6. https://doi.org/10.1159/000329374 PMID:21691055
Greulich W, Pyle I. Radiographic atlas of skeletal development of the hand and wrist. London: Stanford University Press; 1959. https://doi.org/10.1097/00000441-195909000-00030.
Tanner JM, Healy MJ, Goldstein H, Cameron N. Assessment of skeletal maturity and prediction of adult height TW3 method. London: WB Saunders; 2001.
Thodberg HH, Jenni OG, Caflisch J, Ranke MB, Martin DD. Prediction of adult height based on automated determination of bone age. J Clin Endocrinol Metab. 2009 Dec;94(12):4868–74. https://doi.org/10.1210/jc.2009-1429 PMID:19926715
Alshamrani K, Messina F, Offiah AC. Is the Greulich and Pyle atlas applicable to all ethnicities? A systematic review and meta-analysis. Eur Radiol. 2019 Jun;29(6):2910–23. https://doi.org/10.1007/s00330-018-5792-5 PMID:30617474
Michael DJ, Nelson AC. HANDX: a model-based system for automatic segmentation of bones from digital hand radiographs. IEEE Trans Med Imaging. 1989;8(1):64–9. https://doi.org/10.1109/42.20363 PMID:18230501
Pietka E, McNitt-Gray MF, Kuo ML, Huang HK. Computer-assisted phalangeal analysis in skeletal age assessment. IEEE Trans Med Imaging. 1991;10(4):616–20. https://doi.org/10.1109/42.108597 PMID:18222868
Tanner JM, Oshman D, Lindgren G, Grunbaum JA, Elsouki R, Labarthe D. Reliability and validity of computer-assisted estimates of Tanner-Whitehouse skeletal maturity (CASAS): comparison with the manual method. Horm Res. 1994;42(6):288–94. https://doi.org/10.1159/000184211 PMID:7698726
Thodberg HH, Kreiborg S, Juul A, Pedersen KD. The BoneXpert method for automated determination of skeletal maturity. IEEE Trans Med Imaging. 2009 Jan;28(1):52–66. https://doi.org/10.1109/TMI.2008.926067 PMID:19116188
Thodberg HH, Sävendahl L. Validation and reference values of automated bone age determination for four ethnicities. Acad Radiol. 2010 Nov;17(11):1425–32. https://doi.org/10.1016/j.acra.2010.06.007 PMID:20691616
Halabi SS, Prevedello LM, Kalpathy-Cramer J, Mamonov AB, Bilbily A, Cicero M, et al. The RSNA Pediatric Bone Age Machine Learning Challenge. Radiology. 2019 Feb;290(2):498–503. https://doi.org/10.1148/radiol.2018180736 PMID:30480490
Schündeln MM, Marschke L, Bauer JJ, Hauffa PK, Schweiger B, Führer-Sakel D, et al. A Piece of the Puzzle: The Bone Health Index of the BoneXpert Software Reflects Cortical Bone Mineral Density in Pediatric and Adolescent Patients. PLoS One. 2016 Mar;11(3):e0151936. https://doi.org/10.1371/journal.pone.0151936 PMID:27014874
Leijten AD, Hampsink B, Janssen M, Klein WM, Draaisma JM. Can digital X-ray radiogrammetry be an alternative for dual-energy X-ray absorptiometry in the diagnosis of secondary low bone quality in children? Eur J Pediatr. 2019 Sep;178(9):1433–41. https://doi.org/10.1007/s00431-019-03425-5 PMID:31352546
Boeyer ME, Sherwood RJ, Deroche CB, Duren DL. Early Maturity as the New Normal: A Century-long Study of Bone Age. Clin Orthop Relat Res. 2018 Nov;476(11):2112–22. https://doi.org/10.1097/CORR.0000000000000446 PMID:30179948
De Sanctis V, Di Maio S, Soliman AT, Raiola G, Elalaily R, Millimaggi G. Hand X-ray in pediatric endocrinology: skeletal age assessment and beyond. Indian J Endocrinol Metab. 2014 Nov;18(7 Suppl 1):S63–71. https://doi.org/10.4103/2230-8210.145076 PMID:25538880
Zhang SY, Liu G, Ma CG, Han YS, Shen XZ, Xu RL, et al. Automated determination of bone age in a modern chinese population. ISRN Radiol. 2013 Feb;2013:874570. https://doi.org/10.5402/2013/874570 PMID:24967289
Koc U, Taydaş O, Bolu S, Elhan AH, Karakas SP. The Greulich-Pyle and Gilsanz-Ratib atlas method versus automated estimation tool for bone age: a multi-observer agreement study. Jpn J Radiol. 2021 Mar;39(3):267–72. https://doi.org/10.1007/s11604-020-01055-8 PMID:33067733
Alshamrani K, Hewitt A, Offiah AC. Applicability of two bone age assessment methods to children from Saudi Arabia. Clin Radiol. 2020 Feb;75(2):156.e1–9. https://doi.org/10.1016/j.crad.2019.08.029 PMID:31706569
Berst MJ, Dolan L, Bogdanowicz MM, Stevens MA, Chow S, Brandser EA. Effect of knowledge of chronologic age on the variability of pediatric bone age determined using the Greulich and Pyle standards. AJR Am J Roentgenol. 2001 Feb;176(2):507–10. https://doi.org/10.2214/ajr.176.2.1760507 PMID:11159105
Bull RK, Edwards PD, Kemp PM, Fry S, Hughes IA. Bone age assessment: a large scale comparison of the Greulich and Pyle, and Tanner and Whitehouse (TW2) methods. Arch Dis Child. 1999 Aug;81(2):172–3. https://doi.org/10.1136/adc.81.2.172 PMID:10490531
van Rijn RR, Thodberg HH. Bone age assessment: automated techniques coming of age? Acta Radiol. 2013 Nov;54(9):1024–9. https://doi.org/10.1258/ar.2012.120443 PMID:24179234
Lee BD, Lee MS. Automated Bone Age Assessment Using Artificial Intelligence: The Future of Bone Age Assessment. Korean J Radiol. 2021 May;22(5):792–800. https://doi.org/10.3348/kjr.2020.0941 PMID:33569930